True or False: All Antibodies Can Respond to Any Antigen?
Picture your immune system as a highly trained security team, each member equipped with unique skills to tackle specific intruders. But does every guard handle every threat, or are their roles more specialized? antibodies—the body’s microscopic defenders—this question becomes even more fascinating. Can these tiny proteins truly respond to any antigen they encounter, or do they have limits?
Understanding the relationship between antibodies and antigens isn’t just about science; it’s about appreciating how your body protects you daily. The answer might surprise you and could change the way you think about immunity altogether. Let’s unravel this complex yet captivating interplay and uncover whether all antibodies are universal responders—or if nature has designed them with precision for specific targets.
Understanding Antibodies And Antigens
Antibodies and antigens are central to your immune system’s defensive mechanisms. Their interaction determines how effectively your body identifies and neutralizes harmful invaders.
What Are Antibodies?
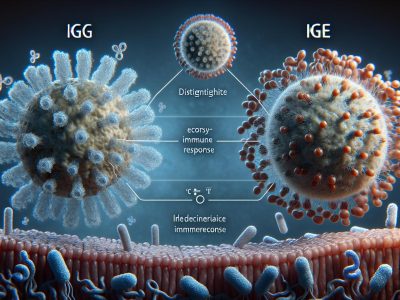
Antibodies, also called immunoglobulins, are Y-shaped proteins produced by B cells in response to specific antigens. Each antibody has a unique structure designed to recognize a particular antigen. For example, IgG antibodies primarily combat viruses and bacteria, while IgE targets allergens.
The variable region of an antibody binds to an antigen’s epitope with precision. This specificity ensures that each antibody responds only to its corresponding target. But, cross-reactivity can occur if one antibody recognizes multiple similar antigens, such as in some autoimmune diseases (e.g., lupus).
The Role Of Antigens In The Immune System
Antigens trigger your immune system by presenting foreign or abnormal structures detectable by antibodies or T cells. These molecules include proteins on pathogens like bacteria or viruses and non-pathogenic substances like pollen or transfused blood types.
Your body’s ability to distinguish self from non-self depends on recognizing these antigens accurately. Pathogens evolve diverse surface proteins (antigenic variation) to evade detection—HIV is an example of this adaptation strategy.
Vaccines use inactivated or weakened forms of antigens from diseases like measles or influenza to train the immune system without causing illness. This controlled exposure helps you build immunity efficiently against future infections caused by the same pathogen.
Exploring The Specificity Of Antibodies
Antibodies interact with antigens through a highly specific mechanism, ensuring targeted immune responses. This section examines whether antibodies can respond to any antigen and highlights the critical role of specificity in their function.
Can Antibodies Respond To Any Antigen?
Antibodies don’t possess the ability to bind universally to all antigens. Each antibody is designed to recognize a specific epitope, which is a distinct portion of an antigen’s structure. For example, IgE antibodies specifically target allergens like pollen or dust mites, while IgM responds primarily during initial pathogen exposure.
Cross-reactivity may occur when structurally similar antigens share epitopes. In such cases, an antibody might mistakenly bind to both its intended target and unrelated molecules. An example is rheumatic fever, where antibodies against Streptococcus bacteria also attack heart tissue due to shared molecular patterns.
The unique variable regions on an antibody’s “arms” determine antigen recognition. Without this precise matching system, your immune defense would struggle against diverse invaders like viruses and toxins.
The Importance Of Antigen-Antibody Binding Specificity
Specificity ensures that immune responses are efficient and non-destructive to healthy tissues. When binding lacks precision, autoimmune disorders can arise as seen in conditions like lupus where self-antigens become targets for the immune system.
Vaccines exploit specificity by introducing harmless forms of pathogens or their components (e.g., protein subunits). These trigger memory B cells to produce tailored antibodies without causing disease symptoms. For instance, the mRNA COVID-19 vaccines instruct cells to create spike proteins mimicking SARS-CoV-2 for antibody generation.
Precise interactions between antigens and antibodies also help diagnostic tools like ELISA tests used in detecting infections or hormonal changes during pregnancy tests.
True Or False: All Antibodies Can Respond To Any Antigen
Antibodies don’t universally respond to all antigens. Their ability to bind depends on the specificity of their structure, tailored for unique antigenic determinants.
Evaluating The Statement
The statement “All antibodies can respond to any antigen” is false. Each antibody is structured to recognize a specific epitope on an antigen. For instance, IgG antibodies target viruses or bacteria, while IgE focuses on allergens like pollen or dust mites. This design ensures that immune responses are both efficient and targeted.
Cross-reactivity serves as an exception where some antibodies mistakenly bind to similar epitopes across different antigens. In autoimmune diseases like lupus, this phenomenon can cause harmful effects, such as the immune system attacking healthy tissues.
Scientific Evidence And Research Findings
Scientific research confirms that antibody-antigen interactions rely on molecular compatibility. A study in Nature Reviews Immunology (2020) described how B cells undergo somatic hypermutation to produce highly specific antibodies during adaptive immunity development.
Vaccines exploit this precision by introducing harmless antigen forms, prompting your immune system to generate pathogen-specific antibodies without causing illness. Diagnostic technologies like ELISA tests further demonstrate how precise these interactions must be for accurate detection of infections or hormonal changes.
Certain pathogens evolve mechanisms like antigenic variation to evade antibody recognition. Influenza viruses rapidly mutate their surface proteins—hemagglutinin and neuraminidase—forcing new vaccine formulations annually due too loss of prior antibody efficacy against novel strains.
Factors Influencing Antibody Responses
Antibody responses depend on various biological and environmental factors. These influences determine their specificity, diversity, and effectiveness in combating antigens.
Genetic Factors And Antibody Diversity
Genetic variation within the immune system shapes antibody diversity. The gene segments encoding antibodies—variable (V), diversity (D), and joining (J) segments—recombine during B cell development to create unique antigen-binding sites. This process, called V(D)J recombination, generates millions of potential antibodies capable of recognizing diverse epitopes.
Somatic hypermutation enhances diversity further by introducing point mutations in the variable region genes after initial antigen exposure. High-affinity clones are selected for proliferation—a process known as affinity maturation. For instance, individuals with defects in AID (activation-induced cytidine deaminase), a critical enzyme for somatic hypermutation, experience reduced antibody efficacy.
Certain genetic factors can also limit this variability. Inherited immunodeficiencies like SCID (severe combined immunodeficiency) impair B cell function, reducing antibody production entirely or partially. Your genetic makeup eventually dictates how well your body adapts to evolving pathogens.
Limitations And Exceptions
Not all antibodies respond effectively to every antigen due to structural constraints and antigenic properties. Each antibody recognizes its specific epitope via the paratope in its variable region; mismatched structures prevent binding altogether.
Pathogens like HIV exploit these limitations by mutating rapidly to escape recognition—a phenomenon termed “antigenic drift.” Similarly, influenza viruses undergo frequent surface protein modifications requiring annual updates to flu vaccines designed against their antigens.
Cross-reactivity represents another limitation where an antibody binds non-target antigens sharing similar epitopes. While cross-reactive antibodies may inadvertently neutralize unrelated pathogens, they risk triggering autoimmune conditions if self-antigens are targeted mistakenly—as seen in lupus or rheumatoid arthritis patients.
Implications For Medicine And Immunology
Understanding the specificity of antibodies reshapes approaches in medicine and immunology. Targeted therapies, such as monoclonal antibodies, rely on this precision to treat diseases like cancer and autoimmune disorders. These therapies use lab-engineered antibodies designed to bind specific antigens on diseased cells without affecting healthy tissues.
Vaccines exemplify the practical application of antibody-antigen specificity. By introducing harmless antigens, vaccines stimulate your immune system to produce precise antibodies that provide long-term protection against pathogens like measles or polio. If antigenic variation occurs, such as with influenza viruses, vaccine updates are required to maintain efficacy.
In diagnostics, tools like ELISA tests depend on the exact binding between antigens and antibodies. This principle enables accurate detection of infections (e.g., HIV) or monitoring conditions like hormonal imbalances in pregnancy tests.
Antibody engineering pushes innovation boundaries in immunotherapy. Bispecific T-cell engagers (BiTEs) combine two distinct binding sites, enabling simultaneous targeting of cancer cells and activation of immune cells for a coordinated response.
The concept of cross-reactivity carries dual implications for health outcomes. While it sometimes aids immunity by recognizing similar pathogens, it can trigger autoimmune issues where self-proteins become mistaken targets—like in type 1 diabetes or lupus.
Recognizing limitations enhances therapeutic strategies. Pathogens exploiting rapid mutations challenge antibody-based treatments; this includes viruses like HIV escaping recognition through structural changes. Research into broadly neutralizing antibodies addresses these gaps by focusing on conserved viral regions less prone to mutation.
Advancing knowledge about antigen-antibody interactions drives innovations across preventative care, treatment modalities, and diagnostic accuracy while highlighting challenges posed by evolving pathogens and cross-reactive responses.
Conclusion
Understanding the specificity of antibodies is essential for appreciating how your immune system defends against threats. Antibodies aren’t universal responders; they’re finely tuned to target specific antigens, ensuring precise and effective immune responses. This precision not only safeguards your health but also drives innovations in vaccines, diagnostics, and targeted therapies.
The remarkable design of antigen-antibody interactions highlights the complexity and adaptability of your body’s defense mechanisms. As science continues to advance, this knowledge paves the way for breakthroughs in combating diseases, improving treatments, and enhancing preventative care.
by Ellie B, Site Owner / Publisher